TMAU (Trimethylaminuria): The Causes, Types and Triggers
TMAU is an acronym for trimethylaminuria, a metabolic disorder characterized by body odor that has a fish smell to it. It was formerly called Fish Odor Syndrome. It is not due to a lack of hygiene. Many cases have been identified with no malodor at all. An estimated 7% of people have an inability to perceive the odor.
The Causes and Types of TMAU
TMAU is caused by the accumulation of trimethylamine (TMA) in body fluids such as urine, sweat, saliva and reproductive fluids. Such accumulation can result in body odor and bad breath and can be quite distressing to people with the disorder. The accumulation occurs because the amount of trimethylamine (TMA), a smelly substance acquired from the diet, is not efficiently converted in the liver to the non-odorous substance TMAO (which is under fire for possible cardiovascular-disease connections). While once considered to be rare, the condition is now said by researchers to be uncommon.
There are two main types of trimethylaminuria: primary and secondary. Primary trimethylaminuria comprises the majority of the reported cases and is inherited in an autosomal recessive way, meaning having two copies of the recessive abnormal genes. The disorder is not confined to one ethnicity. Carriers of only one gene mutation are usually asymptomatic. Primary trimethylaminuria sufferers have an inherited enzyme deficiency of the liver enzyme FMO3 (flavin-containing monooxygenase 3) from a gene mutation.
As of 2011, more than 300 variants or single nucleotide polymorphisms (SNPs) have been found in the gene, and of those, over 40 have been associated with trimethylaminuria. Thus, not all genetic defects in the gene result in this disorder.
Secondary (acquired) trimethylaminuria, or TMAU2, may have associated genetic inactivating mutations of the gene associated with it, and/or it may be the result of some dietary, hormonal or environmental triggers and factors.
These triggers and factors include:
- Age, specifically childhood
- Sex hormone fluctuations
- Stress
- Dietary overload
- Disease states
Most times trimethylaminuria is abbreviated as TMAU whether it is the primary or secondary form and that is what I have done on this page.
Childhood
The FMO3 enzyme is first identified in 30% of fetal livers in the first trimester of pregnancy, disappears in the second and third trimesters, but is identified again post-birth. By 9 months of age, the level increases to 8% of adult levels. By 11 years of age the level increases to 20% of the adult level. Even at age 18, the level of FMO3 is still significantly below adult levels.
That is why some babies and children/teens may noticeably have the disorder, but it fades by the time they reach adulthood.
Transient Sex Hormone Fluctuations
TMAU is more common in women than in men. Symptoms in women can worsen just before and during menstrual periods, after taking oral contraceptives (birth control pills) and around menopause. The exact mechanism for why TMAU would be worse is unknown, but naturally is suspected to be due to fluctuations in sex hormones.
Transient Stress
Anecdotal stories on the Internet relate that during periods of higher stress the trimethylaminuria is worse. This is not hard to imagine as stress can result in a person sweating. Also, stress can disrupt digestion and upset blood sugar levels, hormone levels, gastrointestinal microbiota and many other body functions.
Dietary Overload
If a person consumes too many TMAs or other aggravating foods or has gut dysbiosis, then this exceeds the liver’s ability to oxidize the TMA to TMAO and their body’s ability to handle the excess. More information about dietary issues is provided below.
Disease States
Disease states such as viral hepatitis or a kidney or liver
disease can impair the production of the FMO3 enzyme. They are not the only states which can cause problems for TMAU, however, as I will discuss later.
Since this is a site about probiotics, I want to focus on the dietary overload and disease states aspects of trimethylaminuria starting with where TMA comes from.
What Are Dietary Sources of Trimethylamine?
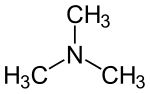 |
Trimethylamine is a molecule containing three methyl (CH3) groups on a nitrogen atom. It is the breakdown product in your gastrointestinal (GI) tract predominantly from carnitine (KAR-ni-teen), choline (KOE-leen), phosphatidylcholine, betaine (BEET-ah-een) and TMAO that are in many foods, supplements and drinks you may consume and that all contain TMA as part of their structure. |
Interestingly, trimethylamine is reported by the National Human Genome Institute to be high in milk obtained from wheat-fed cows.
Carnitine is found naturally in red meats and is added to many exercise powders and energy supplements. Carnitine’s main role is to transport long-chain fatty acids from the cytosol in a cell to the mitochondria (or energy-generating powerhouses) for energy production.
Phosphatidylcholine is found predominantly in foods like eggs, liver, soybeans and soy products, lecithin, mustard, whole grains, legumes such as peas, beans and peanuts, red meats like steak, eggs, energy drinks, some diet supplements, marine life, and many seeds and oils.
Choline is a component of phosphatidylcholine but it is also found alone. Free choline is found in higher amounts in whole grains, liver, soy, collard greens, cruciferous vegetables, some beans and in lower amounts in nearly every spice, herb and food. That also means that choline is found in many of the processed cereals that you may eat every day.
Betaine is found in high concentrations in quinoa, beets, spinach, some supplements and many of the processed, boxed cereals that you may eat that are based on grains. It helps protect many plants from stress so you will find it widespread in nearly everything you eat. Betaine is also a breakdown product of choline between choline and TMA.
Some people have issues with tyramine which is found in aged cheeses, smoked fish, cured meats like lunchmeats and hot dogs, some beers, old leftovers and some fermented foods and drinks. Interestingly, tyramine does not contain the 3 methyl groups characteristic of TMA.
TMAO (an acronym for trimethylamine-N-oxide) is found preformed naturally in seafood. Lower amounts are found in freshwater fish.
Carnitine, choline, phosphatidylcholine and betaine are converted in the body to TMA and then are normally supposed to be converted by the FMO3 enzyme to TMAO. In non-trimethylaminuria sufferers, more than 95% of TMA is oxidized into TMAO by the enzyme.
Since this is a site about probiotics, I still want to focus on the dietary overload and disease states aspects of trimethylaminuria discussing whether or not you should eliminate food that aggravate TMAU and if probiotics can help with this condition. For that information, see this page.
To read about TMAO, click here.
Return to the Homepage.
I research studies and share my clinical experience to write this free site to help you find solutions to your problems. As part of that, I recommend products and services that I genuinely believe will be of help to you. If you click on a link to a product/service, I may receive a small commission to support my efforts if you buy something. The item does not cost you more.
Thanks for visiting this site! If you've enjoyed reading this page or have found the information to be useful to you, please "like", tweet about it, or share it so others can benefit, too. You can leave comments below via Facebook or Disqus.
Comment with Disqus (including as a guest), Twitter or Google accounts:
If you are one of my many readers without a Facebook account, you can still comment.
Disclaimer: Please note: By law, I cannot provide any personalized recommendations for your specific health concern on this site. The information contained in this site is educational in nature and is not intended as diagnosis, treatment, prescription or cure for any physical or mental disease, nor is it intended as a substitute for regular medical care. Consult with your doctor regarding any health or medical concerns you may have.
Subscribe to my occasional newsletter and receive a free copy of "How to Use Probiotics to Lose Weight and Be Healthier".

To comply with the EU's GDPR data privacy regulation, please subscribe here:
Looking for some quality professional supplements, including probiotics? Check out my online dispensary, as I will be doing reviews of some of these products in the future. Click on the Fullscript picture. (Note: If you were a former Wellevate customer, please switch to Fullscript for a better customer experience. Thanks!)
Some competitors of SBI (Solo Build It) are posting fake negative reviews of SBI. If you are considering creating your own website business, or if you have a brick-and-mortar business but want an online presence, I highly recommend SBI!





Comment with Facebook!
I'd love to hear your opinion about what you just read. Leave me a comment in the box below! Other commenting options follow the Facebook comments.